
http://s-media-cache-ak0.pinimg.com/564x/fc/b3/54/fcb354286c669e5687fbe935c9e3156d.jpg
Posted by Deana Whitaker – These eight spices will make any meal lively with an added bonus of faster metabolisms, fat fighting nutrients and more! #Weightloss #Spices
Category Archives: Weight Loss
Yoga Designed For A Flat Tummy!

http://s-media-cache-ak0.pinimg.com/564x/fb/a0/1b/fba01b190041cbcc73f7bfa6afd3b7fe.jpg
Posted by Sheila Thomas – You don’t need to love yoga to bust through this flow. Designed to flatten and tone your tummy, it will require strength and attention. #Weightloss #Yoga
Essential Yoga Stretches For Tight Hips

http://s-media-cache-ak0.pinimg.com/564x/10/c5/11/10c51144967d8ef0b3d2816f866725f8.jpg
Posted by Linley Kirian – Including quick workouts, smoothie recipes, pre-workout snack ideas, yoga, how to become a runner, and more. #Weightloss #Yoga
Yoga Poses for a Strong Upper Body

http://s-media-cache-ak0.pinimg.com/564x/5a/de/59/5ade594c04c24b1ae0133a5b9e9738fa.jpg
Posted by Luz Adriana – Yogaworks instructor Patti Quintero is here to offer up her favorite yoga poses for a strong upper body to challenge you in under 15… #Weightloss #Yoga
Symptoms Of Gluten Related Celiac Disease

https://s-media-cache-ak0.pinimg.com/564x/b6/ab/55/b6ab5514200ba959e35f8a0e5ce748dd.jpg
Posted by Veronica Joiner – Here is some information on the Symptoms of Celiac Disease
If you suffer from any of these symptoms or believe you may be at risk for Celiac disease, please contact your doctor for testing.
1. No Symptoms
Unfortunately, many people who suffer from Celiac disease have no symptoms. This is particularly dangerous as intestinal damage can occur even when no symptoms are present. With new screening techniques, people are being diagnosed without ever suspecting they have the disease. It is important for people with no symptoms but a positive diagnosis to eat properly, as they are still at risk for serious complications of Celiac disease, such as cancer.
2. Bloating
Many people who have Celiac disease suffer from painful bloating. For days after consuming gluten, the stomach may be distended and filled with gas. This can be quite painful. Many people complain of intestinal pain and the feeling of being “6 months pregnant”. They may also suffer from excessive gas and flatulence. Bloating can be symptoms of other dietary conditions, so look for it in conjunction with the consumption of gluten.
3. Diarrhea
Chronic diarrhea is a common symptom of those afflicted with Celiac disease. The episodes may be smelly, explosive, and painful. The color of the stool may be pale or white, and typically floats on the surface of the water. Even solid stools may present these conditions. Related symptoms to chronic diarrhea include hemorrhoids. These can occur when there is not enough substance in the stools.
4. Constipation
While diarrhea is common in Celiac sufferers, some people may be afflicted with constipation. This if from the body sluggishly moving the contents of the bowels. The body may be trying to pull all the nutrients possible from the food as the damaged villi will not work as efficiently. The constipation may be marked by periods of heavy diarrhea as the person consumes gluten. The constipation may cause pain and bloating.
5. Weight Loss or Gain
Many people who suffer from Celiac disease lose weight as their body reacts to the missing nutrients. The diarrhea caused by gluten may stall the absorption of calories from the food, purging the body from its fuel. Conversely, a sufferer may in fact gain weight instead of lose it. Their bodies may be screaming for nutrients, so they eat in excess to achieve proper nutrition. They may have a hard time losing weight until they restrict gluten from their diet.
6. Fatigue
Fatigue is a common complaint of those affected by Celiac disease. Undiagnosed Celiac suffers may have their bodies suffer from malnutrition caused by absorption issues. Their body will respond with extreme fatigue and malaise in response. They may crave sugary foods and drink excessive caffeine just to stay energized. After diagnosis and the removal of gluten from the diet, fatigue may be the first symptom to be eliminated.
7. Trouble Concentrating
People who suffer from Celiac disease may experience something called a “brain fog” in relation to the consumption of gluten. This symptom exhibits immediately after eating gluten and can persist for days. The feeling that it gives is confusion, trouble concentrating, and short term memory loss. A sufferer may forget to pick your children up from school, or even forget what they are writing mid sentence. Thankfully, this symptom does not persist as a person removes gluten from their diet. It may even make them feel finally awake after years of fogginess.
8. Problems Falling and Staying Asleep
Recent studies have found that patients with Celiac disease commonly suffer from disordered sleeping, regardless of if the rest of their diet is healthy or not. Sleep disorders are more common to those suffering from Celiac disease vs. the rest of the general population. The disordered sleeping can be shown through an inability to fall asleep, and being unable to stay asleep. The study found that the causes of the inability to sleep well include depression, fatigue, and anxiety.
9. Numbness and Tingling
Many Celiac sufferers exhibit neuropathic symptoms. Problems with the neuropathic system can affect gross and fine motor control and sensory nerves. An undiagnosed Celiac disease sufferer my find their extremities exhibit nerve problems. This can include a tingling sensation in the hands and feet, ranging from mild to “fallen asleep”. Conversely, they may not feel anything in their hands and feet, as numbness is a common complaint. Other parts of the body may be affected, such as the facial muscles and body nerves.
10. Depression
Unfortunately, depression and suicide rates are higher in people with Celiac disease. Studies have found that even eating a gluten free diet, the rates of depression are much higher than the general population. One study found a connection between disordered eating and depression in women who suffer from celiac disease. As they closely monitor their foods for gluten, disordered and restrictive eating can develop. For suicide risk, it seems that once diagnosed and with dietary changes, the suicide risk is greatly reduced.
Do You Have A Nutrient Deficiency?

http://s-media-cache-ak0.pinimg.com/564x/b0/ae/2f/b0ae2f1a399db65a1912877b42c30c4c.jpg
Posted by Brenda Hughes – 7 Common Signs of Nutrient Deficiency
Look for stunted growth. If a child is not getting enough nutrients, they will not grow at a normal rate. The rate of growth for a particular child varies with their age. For instance, most people grow rapidly from infants to toddlers, then slow their growth until puberty, when they experience another period of rapid growth. If your child does not grow rapidly during these sensitive periods, they might be suffering a nutrient deficit.
- See a doctor regularly to ensure your child is growing at a normal rate.
Check dental health. Inflammation of the gums, especially, is an early indicator of periodontal disease, which may in turn indicate a nutrient deficit. If your gums are puffy, red, tender, and bleed when you floss or brush, you might not be getting enough nutrients. In advanced cases, you might have loose teeth. See a dentist if you experience any of these dental problems.
- See a dentist at least twice each year for a regular dental checkup. Your dentist will be able to refer you to a nutritionist if they believe it is necessary.
Monitor for increased illnesses. People who do not receive adequate levels of nutrients are more prone to colds and viral infections. A nutrient-deficient immune system cannot fight off illnesses that a healthy one can, leading to a greater frequency of illnesses, more severe illnesses, or both. Nutrient-deficient people might, for instance, experience:
- a sore throat
- coughing
- fever
- sneezing
- a runny nose
- fever
- other respiratory tract infections (like pneumonia and bronchitis) and flu-like symptoms
Look for muscle spasms. Muscle spasms are any involuntary contraction or vibration of the muscle tissue. If you suddenly develop facial tics – for instance, a sudden upturning of the mouth, or scrunching up of the nose – you might be nutrient deficient. Eye twitches (closing your eyes with excess force or experiencing difficulty in keeping your eyelids stable) could also indicate you need more nutrients. Painful cramps in your legs (especially your calves or thighs) are also reported in some cases of nutrient deficits.
- You might be experiencing a magnesium deficit, since magnesium helps regulate the neuromuscular system that allows our muscles to relax.
- Deficits of B vitamins and calcium might also contribute to muscle spasms.
Look for thyroid problems. Some kinds of nutrient deficiencies – especially iodine deficiency – lead to imbalances in the thyroid and an inability to produce and regulate hormones properly. Signs that your thyroid might be acting up include weight gain, deceased libido, goiter (swelling of the thyroid gland that usually produces a large bump in the neck), hair loss, and infertility
Look for eye problems. In a developing child, a vitamin A deficit could lead to blindness or visual impairment. If your child cannot see well, or suffer from night blindness (an inability to see in the dark), they might not be getting enough vitamin A. Other eye problems like cataracts and macular degeneration also occur in people who have a deficit of vitamin C, vitamin E, zeaxanthin, and zinc.
- You can detect macular degeneration and cataracts by paying attention to any loss of quality in your vision. Blurriness, clouded vision, and increased sensitivity to light are common symptoms.
Look for signs of malnutrition. Nutrient deficiencies are one form of malnutrition. Signs of this condition include, notably, sunken eyes and a bony frame with visible ribs. The skin of a nutrient deficient person will be leathery, dry, and inelastic. Jaundice (yellowing skin) could also occur. Finally, a malnourished person will usually feel lethargic and have low energy levels overall.
- Malnutrition usually indicates that someone is not getting enough calories or is not getting a balanced diet. Malnutrition might also indicate that someone is getting too many calories.
See a doctor. The many symptoms of nutrient deficits are common in many other conditions and diseases. Therefore, in order to rule out other possibilities, it is important to see a doctor and get a professional diagnosis of your condition. Doctors can draw and analyze your blood to determine concentrations of key nutrients. Some doctors might conduct a cellular analysis as well as (or instead of) a blood analysis. If you suspect you or your child has a nutrient deficit, see a doctor and explain why you’re concerned about your nutrient levels.
- Your doctors might not need to conduct a blood analysis if signs and symptoms of a nutrient deficit are obvious enough.
- Your doctor might run tests to look for levels of specific nutrients, or just do a general screening for major nutrients.
You Are More Bacteria Than Human!
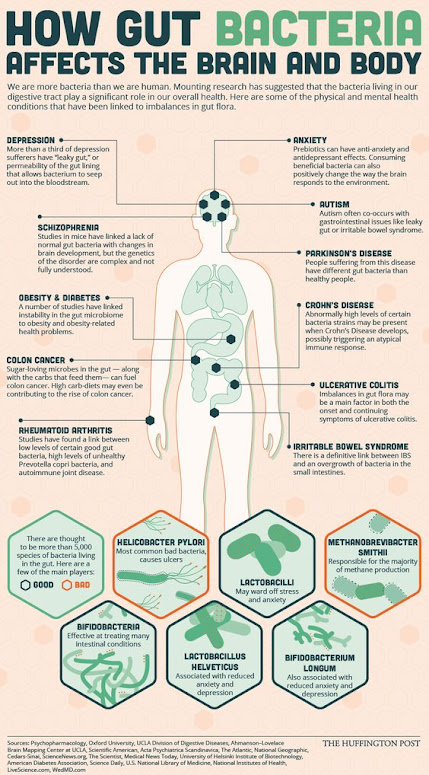
Posted by Grammy B – Advances in Medicine and Biology – #Probiotics #GutBacteria
Microbes Outnumber Human Cells
You’ve probably heard that microbe populations living in and on our bodies outnumber our human cells 10:1. While this ratio is in dispute (some researchers suggest that its more like 1.3:1, the fact remains that the average human hosts about 100 trillion microbes and, even with the more conservative estimate, outnumber human cells.
The Human Microbiome
The human microbiome are the bacteria, viruses and fungi that live everywhere in the body, including on the skin, and inside the mouth and nose.
The Gut Microbiome
The microbes living in the intestines (i.e., the gut) and their role in human health, illness and chronic disease have been the subject of many recent and ongoing scientific research.
Based on the findings, it is now widely thought and accepted by leading experts in the health professions that an imbalance in the gut microbiome can lead or contribute to many different health conditions, illnesses and diseases (as illustrated in this Infographic) including anxiety, autism, depression, Crohn’s Disease, Parkinson’s Disease, schizophrenia, rheumatoid arthritis, ulcertative colitis, Irritable Bowel Syndrome (IBS), obesity, diabetes and certain cancers.
An “imbalance” that is linked to adverse health consequences usually means an overgrowth of “bad” bacteria like H Pylori, or yeast, like Candida Albicans.
This infographic illustrates just a few of the “good” and “bad” bacteria that are known to live in the human intestine.
Plantar fasciitis exercises

http://s-media-cache-ak0.pinimg.com/564x/06/b8/e9/06b8e95392cc1302931281bb1b5c23b8.jpg
Posted by Sophie McCauey – Plantar fasciitis exercises
Roughly 10 percent of the adult population suffers from the type of heel pain known as plantar fasciitis. (1) Plantar fasciitis is caused by inflammation of the thick fascia tissues of the heels. It’s a common running injury and usually triggered due to overuse of the feet during exercise, or from working out with poor form. It can affect either one heel at a time (usually in the dominant foot), or both simultaneously.
Facts About Plantar Fasciitis:
- Plantar fasciitis is the most common cause of heel pain in adults. It accounts for an average of one million patient visits per year to family doctors, orthopedics and general surgeons
- Experts believe that the causes of plantar fasciitis are multi-factorial. Risk factors include overtraining, older age, excessive foot pronation, obesity or being overweight and poor form when working out
- It’s most likely to affect middle-aged people and those who spend lots of time on their feet or exercising. In fact, about 83 percent of patients with heel pains are active working adults between the ages of 25 and 65 years old
- Athletes (especially runners), people who have physically-demanding jobs and soldiers are most susceptible to developing heel problems and pains
- The prevalence rates of plantar fasciitis among runners is between 4 to 22 percent, with higher rates occurring in those who don’t allow enough time between workouts for proper muscle recovery
- Studies show that about one-third of all people with plantar fasciitis report experiencing painful symptoms in both feet
- According to the American Academy of Orthopedic Surgeons, more than 90 percent of all patients with plantar fasciitis will improve within 10 months of starting simple treatment methods which can be done at home (2)
5 Plantar Fasciitis Natural Treatments
For the majority of people with plantar fasciitis, conservative treatments — as opposed to more aggressive treatments like surgery, shock wave therapy or steroid injections — can help decrease inflammation and pain.
1. Rest, Massage & Ice the Heel
The first order of business in treating plantar fasciitis involves taking time off from repetitive movements that trigger the condition and increase pain. You’ll likely need at least several weeks of rest to allow the affected tissue to heal properly, although the exact time period needed differs from person to person. While you’re giving your feet a rest, you can continue to perform low-impact sports that don’t cause pain, including swimming or bicycling.
Immediately after an injury or episode that causes swelling, icing can be helpful. Try elevating the affected foot and applying an ice pack for 15 to 20 minutes, 2 to 4 times daily. Some experts even recommend freezing a water-filled paper cup and rolling it over the site of discomfort for about five to seven minutes to massage the area. (3)
Once swelling subsides a bit after about 2 to 3 days, massage the heel and apply heat along with beneficial essential oils to further reduce inflammation. Warm oil massages are extremely beneficial for your feet because they increase blood and fluid flow, speed up the healing process and break up scar tissue or adhesions that can harden. Massage the painful heel with your hands in circular motions for 15 minutes or more daily. Try warming up a small amount of coconut or olive oil and then adding essential oils like rosemary oil, thyme oil, rose oil or lavender oil to decrease pain and swelling.
2. Practice Heel Exercises and Stretches
Studies show that in patients with plantar fasciitis, stretching exercises for the legs and affected heel are one of the most effective treatment options. Stretching the bottom of the foot, along with exercising and strengthening the legs (especially the calf and Achilles tendon), reduces tissue adhesion, improves form, helps improve range of motion and may decrease pain.
One study from the Baltalimanı Osteopathic Training and Research Hospital in Turkey found that 96 percent of patients with plantar fasciitis experienced improvements after performing specific heel stretches for 5 months. The study also found that symptoms improved after performing stretching exercises twice a day. Stretches included 10 repititions, holding for 20 seconds each time. The American Orthopedic Food And Ankle Society, along with the Mayo Clinic, recommend the following exercises and stretches to help treat plantar fasciitis: (3, 4)
- Towel stretches: Pull on both ends of a rolled towel that you place under the ball of your foot. Move your foot and the towel around to help massage the affected tissue. You can use a warmed towel for extra relief.
- Toe stretching: Cross your affected leg over your other leg and take hold of your affected foot. Pull your toes back towards your shin. Hold this stretch for 10 seconds and do 10 repetitions.
- Thumb massage: Try rubbing your thumb left to right over the arch of the affected foot. As healing progresses, the tissue will ideally become firm like a guitar string.
- Squat stretches: Lean forward and spread your feet apart with one foot in front of the other. Flex your knees and squat down, keeping your heels on the ground as long as possible. Hold for 10 seconds at a time. Repeat 20 times.
- Achilles tendon stretches: Place your affected leg behind your unaffected leg with the toes of your back foot pointed towards the heel of your other foot. Lean against a wall and bend your front knee while keeping your back leg straight. Keep your back heel firmly on the ground and stretch it for 10 seconds at a time, up to 10 times daily.
3. Wear Supportive Shoes & Footwear
Your shoes can really impact your walking or running form. Shoes also impact your ability to withstand force and pressure. If you experience heel pain frequently, it’s a good idea to consult an expert, such as a physical therapist or trained employee in a sporting goods store. They can measure your feet and help you find the best type of sneakers or shoes for your foot type. Your shoes can offer extra cushion and arch support which lower risk for injury while exercises or going about your day. (5)
If you’re a runner, make sure to buy new shoes after about 500 miles of use to avoid wear-out and injury. Avoiding high heels, sandals and going barefoot on hard surfaces can all help control heel pains and symptoms. Another option would be to consider to wearing specialized foot orthotics or splints. Your doctor or physical therapist might recommend wearing a splint that stretches your calf and the arch of your foot. These can even be worn during sleep without much effort at all (called a “night splint”). Night splints help keep the plantar fascia and Achilles tendon in a lengthened position which increases flexibility. Heel cups are another useful support device, made of cushions that are custom-fitted to your arches in order distribute pressure to your feet more evenly.
4. Maintain A Healthy Weight
Reaching and sustaining a healthy body weight (meaning a BMI between about 19 to 25 for most people) can help minimize the amount of stress placed on your heels. The higher your body weight, and the weaker your lower leg muscles, the more pressure your heels experience. (6)
Eating an anti-inflammatory diet, reducing stress, getting enough sleep and regularly exercising can all help with weight loss and maintenance. Some of the best foods for weight loss and controlling inflammation include: fresh fruits and vegetables (these are rich in magnesium and potassium), raw foods, green juices, wild-caught fish, probiotic foods, nuts and seeds, and healthy proteins like cage-free eggs and pasture-raised poultry. Just be sure to choose organic produce to avoid the dirty dozen.
5. Consider Visiting a Physical Therapist
If pain doesn’t subside after following the advice above on your own, visit a physical therapist. A therapist teach you how to perform heel exercises to stretch the plantar fascia in the most effective way. If you’re new to running or exercising, a therapist can also work with you to learn proper form. Therapists can also help you learn how to strengthen your Achilles tendons, calves and lower leg muscles, along with your ankles and lower back, to stabilize your body weight over your heels better.
10 Smoothie Recipes For Weightloss!

http://s-media-cache-ak0.pinimg.com/564x/0f/74/85/0f7485830572d5af3556e6aede4d1908.jpg
Posted by Loteba Soto – The nutritious & delicious way of losing fat is by including smoothies. Shed your excess belly fat by just sipping in these weight loss Smoothies! #Weightloss #Smoothies #Recipes
Is Your Green Smoothie Even Healthy?

https://s-media-cache-ak0.pinimg.com/736x/57/40/21/57402118e236a31cdada6e6be5b43ff5.jpg
Wake, smoothie, move, repeat. Wake, smoothie, move, repeat.
Green juices or smoothies have become part of everyday vernacular, almost as ubiquitous as a daily caffeine hit, among the health conscious anyway. But despite nutritious smoothies being a buzzword for years now (green smoothie is one of the biggest “trending” words in 2015), its widespread fame hasn’t changed the fact it’s rare for daily greens to be well executed.
And, here’s the clincher, because of this, it actually has little or none of the desired effects on your health and energy.
GREEN BENEFITS
It’s touted as your daily equaliser, an input of nutrient dense and enzyme-rich liquid that can help make you feel great and perhaps help you look it too. It has the potential to deliver easily accessible nutrition to your system and can help you detoxify. If your health is in “credit”, then a green smoothie/juice can further create a bit of a buffer to nutritional and life stresses.
While the idea of grabbing a pre-mixed or pre-powdered greens together with a new, trendy milk or “mylk”, appears to be an efficient way of throwing in the good stuff while getting optimum benefits, the truth is it probably isn’t. There are improvements to be made, and lots of them.
GREEN SMOOTHIE MISTAKES
1. Using pre-mixed, pre-powdered greens and berries
There are an abundance of these fruits and vegetables in their fresh and whole form, with all their intact enzymes and catalysts at your local growers market. A minimal amount of dead, dried, pesticide and chemical farmed green powder is not of any benefit to anyone. Always go fresh when you can.
2. Using low-grade protein powder
Putting awesome fresh produce in your shake and then degrading it by adding a low-grade protein source is not the best way to go.
You’re potentially adding a whole bunch of hidden fillers, inflammatory agents or chemicals to what is supposed to be our remedy against these things! Look out for ingredients like colourings, preservatives and a list of inactive ingredients longer than the active ingredients.
3. Check your superfood blend
Adding superfood blends that only contain micro-doses of the superfoods that you were after is commonplace. Have you considered how much you are going to actually need of that exotic sounding “superfood”?
Some brands contain only contain one tenth or one hundredth of the star ingredient they are promoting, which will do little for your health, even though they are listed on the label and are a selling point for the product.
4. What’s your pre-made blend made of?
Using pre-made blends that have added ingredients for texture, consistency and shelf life need to be scrutinised closely.
Ingredients to avoid are inactive ingredients – they’re inactive because they haven’t been added for use in the nutritional content of the product, but are still put in the product, which means your body still has to process and deal with it.
While some natural sweeteners are OK, again without sourcing them yourself you have little control over their quality. Other sweeteners are flat out terrible for your system – high fructose corn syrup and maltodextrin are the big ones to look out for so avoid these at all costs.
GREEN SMOOTHIES COME GOOD
The main point is, we need to start questioning all ingredients. It doesn’t help anyone if the “healthy” ingredients are produced in an unhealthy way, with unhealthy fillers. The benefits and assurance of using some home ingredients like a quality honey, or some well sourced stevia are more beneficial and harmonious to your body.
The other thing to look out for is food derived from a wholefood.
Most of the beneficial elements, such as vitamins and minerals, found in wholefoods are only used by the body when consumed with the rest of the wholefood. A wholefood contains the needed catalysts and enzymes to help you break down and make use of the nutrients you need to get out of those healthy foods. Nature has already got a great system set up for us and unfortunately separating and prepackaging parts of the wholefood, or synthetically trying to recreate elements of it doesn’t necessarily work.
Yes, it’s a smoothie ingredient minefield out there!
HOW TO MAKE THE BEST GREEN SMOOTHIE POSSIBLE
1. Buy fresh, quality produce
Preferably from local markets or growers. This way you know (because you can ask) where your fruit and veg has been, how long it has (or hasn’t) been in storage and what sort of conditions it has been grown in. Go chemical-free, organic, and sustainably grown produce. Buy lots of it and buy variety.
We recommend a variety of colours and particular qualities (for example, avocado for fat, banana for potassium, etc). Mix it up, too; the number of documented benefits to a wide variety of fruit and veg is only made to look dull by the potentials, uses and benefits we haven’t discovered yet.
2. Pick a suspension fluid
All of the produce will be blended into oblivion so you’ll need something liquid to carry them for texture and enjoyment’s sake (even if you are about your hardcore health there’s nothing wrong with having a health dense and tasty smoothie). Try home-made nut milks, hemp milk or coconut water.
3. Pick the right protein
If you are going to add a protein source, or a powder, do your research. Know your products. Do they use proprietary blends? Then guess what – it’s impossible to know what the hidden ingredients are. Are they transparent with the sourcing of their ingredients? If not, why not? Are they traceable sources? There are companies out there making the effort to nail these crucial factors in the products they deliver. It’s worth finding them and using them.
4. Get yourself an easy to clean, simple blender
You will make the money back on the cash you don’t spend on pre-packed, potentially low quality juices, and you will hit more variety and therefore more nutrition!
Red Hippo, run by Nick Dawe and Mitch and Ryan Barraclough, is an Australian company that provides synergistic protein blends, supported by science, and road tested by Olympians.
